How hybrid learning flourished in health-care programs this term
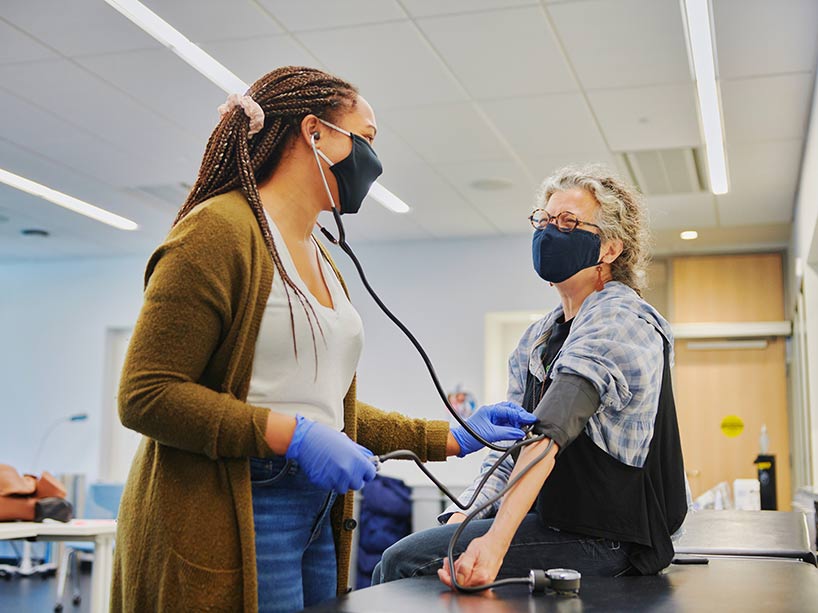
Professor Nicole Bennett, right, acts as a patient for midwifery student Hannah Cole. Cole is one of the students who has been able to return to campus for safe in-person learning this semester. Photo: Alyssa K. Faoro.
As the semester winds down, there is an opportunity to reflect on the incredible amount of effort that has gone into ensuring students are receiving the best possible experience while COVID-19 continues to restrict traditional in-person learning.
The Daphne Cockwell School of Nursing and the Midwifery Education Program within Ryerson’s Faculty of Community Services have adapted in ways that exemplify the hybrid learning model. Both nursing and midwifery are practice disciplines that typically offer valuable in-person learning opportunities. This semester, faculty from both disciplines found ways to safely provide some in-person learning opportunities, while getting creative with remote teaching.
The creativity we’ve seen across campus these past nine months could pave the way for new styles of learning in the future.
Daphne Cockwell School of Nursing
Planning for a safe return to campus started early for Daria Romaniuk, professor and associate director of the Collaborative Nursing Degree Program in the School of Nursing. She and her team started exploring the possibility in June 2020. They were responsible for ensuring that all safety protocols were met while students got valuable lab practice.
“Some things done in the lab could be recreated for students virtually, but not everything. We thought it best to do as much as we could in person,” she said.
Three courses held in-person labs this fall. The content and number of students for each lab is different, so Romaniuk had to figure out plans for each course in order to maintain public health guidelines, including physical distancing and mandatory use of face masks. Students are required to complete a COVID-19 screening questionnaire online before going to campus and the labs are scheduled to be slightly longer so students can come in every other week in order to minimize travel.
The measures allow students to work with the proper equipment and have access to quality coaching, which Romaniuk acknowledges is important for those students who are just starting to hone their nursing skills.
“We want students to get as much of the realistic experience as possible [and] the students appreciate the opportunity to be in the labs,” said Romaniuk. “So long as circumstances are such that we're able to come into the labs, we will come into the lab.”
When it comes to remote learning, Ryerson’s School of Nursing had previous experience, having employed award-winning gamification teaching tools long before the pandemic. Students can access a “virtual hospital” where they can practice patient care in a safe virtual environment at their own pace. Students can access the games at any time as a learning tool, and some games have also been incorporated into course requirements.
“You can't guarantee, even in a clinical setting, that every student will have the kinds of experiences that you want them to have,” said Romaniuk. “The virtual simulation gives us the opportunity to ensure that all students can have the same experience.”
Romaniuk said that since COVID-19 started, she has received requests from other nursing schools across North America to use the games. The virtual health-care experience is available for anyone to use free of charge.
Midwifery Education Program

Professor Nicole Bennett in Ryerson’s Midwifery Education Program credits the faculty for the creative ways they were able to help students learn remotely, including sending students home with a specially-designed “sock arm” for practicing blood samples. Photo: Alyssa K. Faoro.
For professor Nicole Bennett, who teaches a course called Clinical Skills in the Midwifery Education Program, drawing blood, setting an IV and ascertaining a baby’s position are all incredibly important skills to learn in person. In normal circumstances, students spend six hours a week in workshops learning these hands-on skills.
COVID-19 and the shift to remote learning provided an opportunity for creativity. Students were given bags filled with clinical equipment, teaching tools and supplies, which they used during online workshops.
For example, students practised the skills needed to take blood samples remotely. Students normally have access to simulation arms that have imitation veins and students draw imitation blood. To recreate this, Bennett sent the students home with supplies including a "sock arm" which was designed by professor Andrea Roberson. The sock arm is a simple tube sock filled with stuffing and a catheter which helps students practice skills needed to draw blood at home.
While developing tools like this have helped fill the gap, Bennett agrees that there are just some elements of the course work that require in-person learning, specifically the skills assessment.
“We need to be certain that our students have learned enough skill that they could confidently go into their placements and be safe,” she said.
Following the same safety protocols as nursing students, midwifery students have been going to campus for clinical skills assessments that will ensure standards are met before they start their clinical placements.
“With in-person assessments, we were able to do small corrections and provide additional explanations that really helped them,” said Bennett. “So, in as much as I thought we did a good job offering alternatives during remote learning, students very much appreciated the face-to-face interaction.”
A student’s perspective

Nursing and Midwifery students, like Hannah Cole, pictured, were able to return to campus for valuable in-person labs and assessments. Photo: Alyssa K. Faoro.
Hannah Cole is in her second year of the Midwifery Education Program and is in Bennett’s Clinical Skills class. Cole is impressed with how innovative her learning experience has been this semester, giving credit to the kits that were created for each student.
“It was stressful, especially at the beginning, but now that it’s the end of the semester I'm really comfortable with how they managed to transform the whole course. They did a great job and I really don't think it hindered our ability to learn,” she said.
Most in-person assessments have concluded for the semester and professor Bennett is now able to look back on the last few months.
“We’re entering our last classes looking at each other and wondering, how did we pull this off?” she said. “COVID forced us to and we managed.”